Cervical cancer is the second most frequent malignancy in Indian women after breast cancer. Cervical cancer is avoidable because it has a well-defined, protracted pre-malignant period that can be diagnosed by routine screening tests and follow-up. Unfortunately, most Indian women are unaware of the screening. Call and book your appointment with Dr. Amita Shah, the best gynae for women in Gurgaon.
What is cervical cancer?
Cervical cancer is a form of cancer that develops at the lower end of the uterus, where it meets the upper vagina, known as the uterine cervix. Due to a lack of access to screening and immunizations against human papillomaviruses, cervical cancer is a leading cause of death in women in the majority of underdeveloped countries (HPVs).
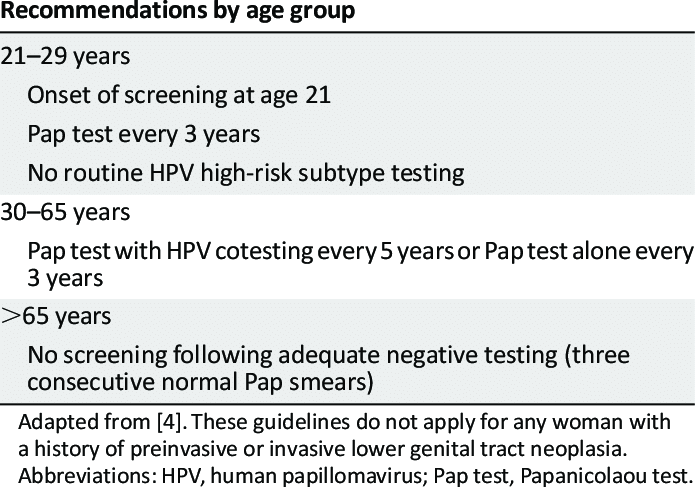


What is the difference between an HPV test, a Pap test, and an HPV/Pap test, according to the ICMR guidelines for cervical cancer screening?
A Pap test, also known as a Pap smear, checks for abnormal cells in the cervix that can lead to cancer. An HPV test detects the human papillomavirus, a virus that can lead to cervical cancer. An HPV/Pap test combines an HPV test with a Pap test.
An HPV test and a Pap test are both performed in the doctor’s office by collecting a sample of cervical cells with a scraper or brush.
For decades, the Pap test has been the gold standard in cervical cancer screening.
HPV testing is a newer form of screening for cervical cancer. The Food and Drug Administration (FDA) has approved two HPV tests for use as primary HPV tests, which means they are not part of an HPV/Pap contest. Other HPV tests are permissible as part of an HPV/Pap contest.
Why does the revised guideline favour an HPV test over a Pap test or an HPV/Pap contest?
Cervical cancer precursors can be detected using any of the three tests. However, research has shown that HPV tests are more accurate and dependable than Pap testing. Also, because HPV tests can rule out disease so effectively, they do not need to be done as frequently.
Although the Pap test has resulted in significant reductions in the rates of cervical cancer and death from the disease, it does have some limitations. Because Pap tests are less sensitive than HPV tests, they may miss some precancers and must be performed regularly.
They also detect a variety of aberrant cell alterations, including some modest changes unrelated to HPV. As a result, many people who have an abnormal Pap test result have a very low risk of developing cervical cancer.
HPV/Pap co-testing is only slightly more sensitive than HPV testing, but it’s less efficient as it involves two tests. It also identifies many minor changes that have a very low chance of developing into cancer. That is a significant additional effort and cost for an entire population.
Screening with an HPV test alone was not recommended in 2012 since the FDA had not yet approved that strategy. As equal choices, the guideline provided HPV testing alone, testing, and Pap testing. The new guidelines differ in that they prioritise HPV testing over the other two tests.
Why does the new guideline propose commencing screening at the age of 25, rather than the age of 21?
Using data from new trials, researchers determined that the advantages of cervical cancer screening may not outweigh the risks for those aged 21 to 24.
This is a significant change linked to HPV vaccinations.
The first group of women who received the HPV vaccine when they were younger are now in their twenties and can be screened for cervical cancer. HPV vaccines are extremely effective at preventing HPV infections, particularly infections with HPV strains 16 and 18, which cause many cervical malignancies. As a result, the immunizations have resulted in a decrease in HPV infections and cervical cancer in this age range.
Furthermore, most HPV infections in young women resolve on their own. Screening persons in this age group frequently results in unneeded therapy, which might have negative consequences. As a result, the ICMR recommends beginning screening at the age of 25.
Have the recommendations for people aged 65 and up changed?
No, the recommendations for this age group remain unchanged. If you have a lengthy history of normal screening test results, you can discontinue screening at the age of 65. If you have had an abnormal result or anything worrisome on a screening test in the past, or if you have had treatment for cervical cancer or precancer, you should continue to be screened.
Over the years, the recommended age limit for cervical cancer screening has remained consistent across different standards. However, there are current initiatives to research age restriction more thoroughly because it is an area with limited data. There is a growing interest in examining people who have an abnormal screening test result at an older age to see whether they need extra years of screening or more frequent screening.
Isn’t it better for patients to get examined more frequently and with more tests if these screening tests save lives?
No. When used too frequently, these tests, like many others, have the potential to cause more harm than good. Cervical cancer screening tests pose some risks.
Physical discomfort may result from screening and follow-up testing. There is also the chance that inaccurate, or false-positive, test results will cause more worry and other emotions. And if your test results are erroneous, you may be subjected to unwanted follow-up testing or even therapy.
Cervical cancer or precancer treatment can permanently damage the cervix. This may increase the likelihood of major difficulties in a future pregnancy, such as miscarriage or premature birth.
Therefore, although testing more frequently or with more tests may seem like a good idea, it can lead to more harm. To update their recommendations, the ICMR thoroughly reviewed the possible benefits and hazards of each screening test for each age group.
Do persons who received the HPV vaccine still need to be screened for cervical cancer?
Yes, the new guideline recommends screening for those who have received the HPV vaccine. It does not suggest making a screening decision based on whether a person has received the vaccine or not.
However, as the rate of HPV vaccination among people eligible for cervical cancer screening rises, we may see additional adjustments in screening guidelines in the future.
Why do cervical cancer screening guidelines constantly change?
It’s a dynamic scenario for a variety of reasons. One is that we have seen incredible benefits from the HPV vaccine, which is constantly changing the picture for screening.
We have also seen significant advancements in new technologies such as HPV testing, as well as improvements in some of the secondary tests used for follow-up after screening.
All these advancements have enabled us to create more precise forecasts of a person’s risk of developing cervical precancer and cancer. We also have fresh evidence from large studies that give us confidence that we can update screening techniques to improve outcomes for women and the health care system.
Call and book your appointment with Dr. Amita Shah, the best gynaecologist in Gurgaon.